Updated 3 days ago
Pre-Analytical Blood Collection: Workflow and Best Practices
sidrahafeez754

Pre-Analytical Blood Collection
Guide to Laboratory Accuracy and Sample Integrity
Laboratory testing is founded on pre-analytical blood collection. It encompasses all the operations that take place before a blood sample gets to the analyzer. This includes preparation of the patient, venipuncture, manipulation, labeling, transportation, and storage of the specimen.
- In modern clinical laboratory diagnostics, the pre-analytical stage of laboratory testing is linked to almost 70 percent of testing errors. This makes it the most important step towards ensuring accuracy and quality in blood sampling.
- It is not a technical process per se. It is procedural, too, and highly sensitive. Any minute mistake in the gathering and handling of the sample may affect the entire laboratory diagnosis process.
Importance of the Pre-Analytical Phase in Blood Testing Accuracy
Blood testing accuracy is dependent on the pre-analytical phase, which is essential and cannot be overemphasized. This measure will ensure that the specimen is a real image of the patient.
The primary purposes of its importance:
- Ensures the integrity of specimens.
- Reduces pre-analytical variability of lab tests.
- Precludes failure of diagnostic error reduction measures.
- Meets the requirements of medical laboratory science.
- Enhances the accuracy of healthcare diagnosis.
When this is properly managed, the laboratories are more dependable, faster in diagnosis, and patient outcomes are enhanced.
Pre-Analytical Workflow in Laboratories
Laboratory pre-analytical workflow is a collection of structured processes that ensure the quality of samples during collection and processing.
Key steps include:
- Patient identification and preparation.
- Venipuncture pre-analytical steps
- Blood specimen collection methods.
- Labeling and identification of samples.
Transport and Storage Conditions of Samples
- Sample preparation and centrifugation.
- Separating serum and plasma.
The hospital blood collection procedures should be followed in all steps to avoid errors and be uniform.
Phlebotomy in Healthcare
Phlebotomy plays an important role in phlebotomy pre-analytical procedures. It entails experience, precision, and precautions.
The usual phlebotomy practices are:
• Patient preparation before blood draw.
• Time of tourniquet use.
• Aseptic blood collection method.
• Phlebotomy draw-in sequence.
• Proper blood sample collection methods.
• The vacuum blood collection system uses pre-analytical.
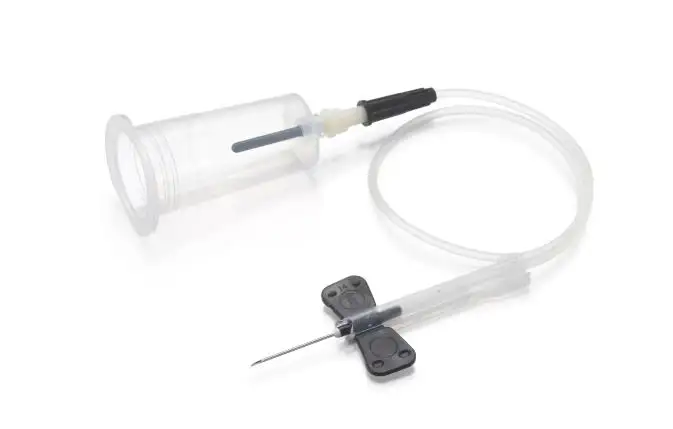
Advanced methods, such as the butterfly needle blood collection method and capillary blood sampling methods, are used to deal with difficult cases. The practices ensure that the blood specimen collection process is accurate and reduces the chances of contamination.
Pre-Analytical Variables in Blood Collection
Blood collection has several pre-analytical variables that may affect the test results.
These include:
- Patient position at the time of collection.
- Sample collection time.
- Status of exercise or fasting.
- Anticoagulants in blood tubes.
- Environmental temperature
- Delay in transport
These are the variables that directly affect the outcomes of laboratory testing at the pre-analytical stage. These should be managed adequately to ensure that there is better specimen management in the pre-analytical phase and a reduction of variability.
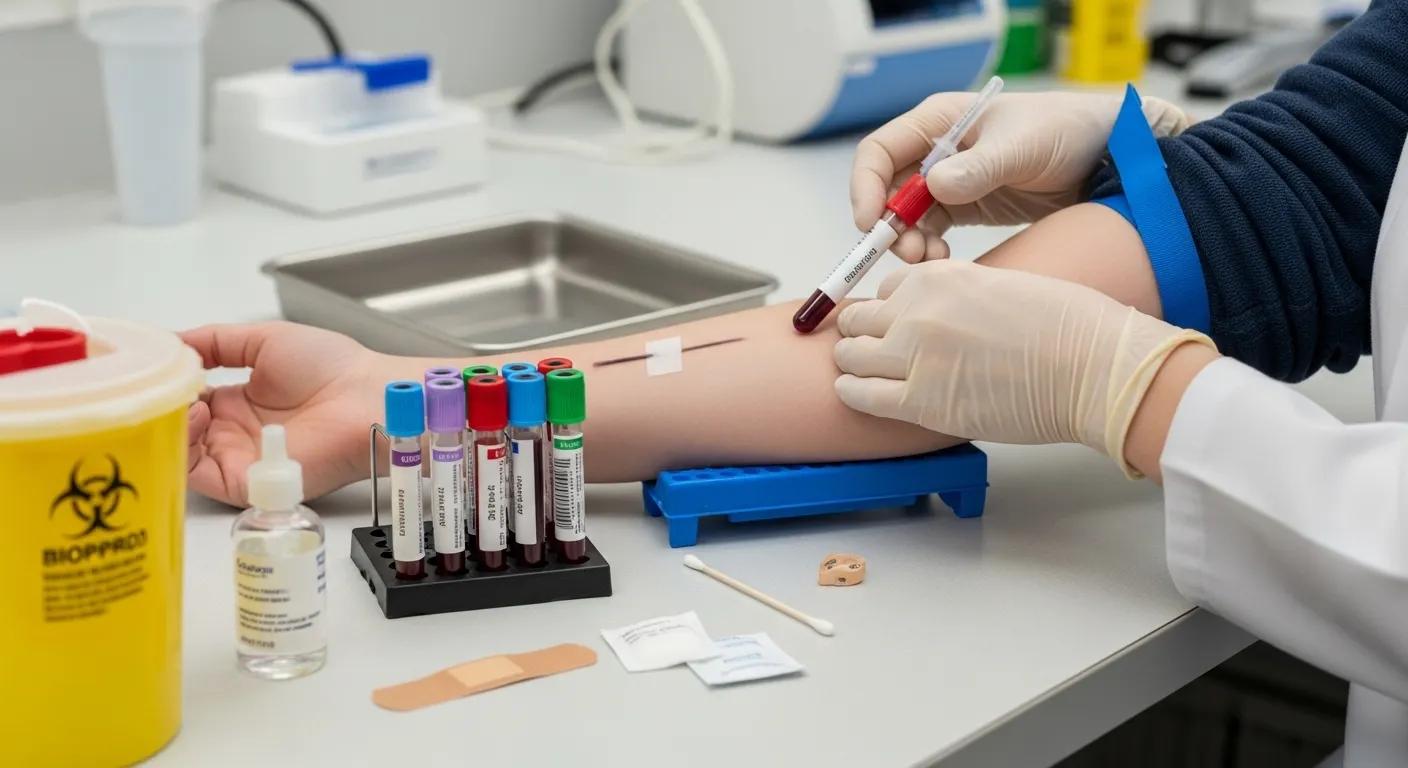
Pre-Analytical Blood Collection Errors and Their Consequences
Pre-analytical errors in the collection of blood are the most frequent sources of inaccurate lab results.
Common issues include:
• Blood sample hemolysis.
• Pollution of the samples during the blood collection.
• Mislabeling blood samples.
• Development of blood clots in samples.
• Reason for specimen rejection: laboratory.
Such misdiagnoses can lead to late treatment and increased medical costs. The effects of pre-analytical errors on laboratory results should be known to improve quality systems.
Causes of Hemolysis and Sample Contamination
One of the most common lab issues is hemolysis. Blood samples cause hemolysis due to:
• Excessive force during a venipuncture.
• Improper needle size
• Shaking of blood vessels.
• Delayed processing
• Temperature fluctuations
Similarly, poor aseptic technique and mishandling of collection devices are also risk factors of sample contamination.
Pre-Analytical Blood Collection Procedures: Quality Control
Clinical laboratory quality control ensures consistency and reliability of results.
Significant quality indicators are:
• Standard operating procedures (SOPs).
• Adherence to ISO 15189 laboratory accreditation.
• CLSI blood collection guidelines.
• Phlebotomy personnel training.
• Regular equipment calibration
• Sample traceability systems
Such systems improve workflow and measures to minimize diagnostic errors.
Pre-Analytical Phase Specimen Handling
Proper manipulation of specimens in the pre-analytical stage ensures that blood samples are in a stable condition and can be utilized.
Important practices include:
• Correct tube selection
• Immediate sample mixing
• Controlled storage conditions
• proximity to laboratory.
Not to be subjected to light or heat. Bio specimen handling procedures should be maintained to maintain biological integrity.
Sample Transport and Storage Conditions
Transport is one of the sensitive factors of the laboratory diagnostic workflow.
Mishandling can lead to:
- Degradation of analyses
- Delayed test results
- False readings
Best practices include:
- Temperature-controlled transport
- Secure packaging
- Timely delivery
- Chain of custody records.
Application of Sodium Citrate Tube in Blood Collection
One of the important components of coagulation testing is the sodium citrate tube. It plays a role in stabilizing the samples. The roles of the sodium citrate tube are:
• Anticoagulant.
• Stores plasma that is to be used in coagulation tests.
• Maintains calcium in check in the sample.
• Ensures that clotting time is measured correctly.
This tube is widely used in clinical pathology practice and hospital laboratory diagnostics in the sphere of coagulation testing.
Laboratory Sample Handling Standards Diagnostic
The modern laboratories are informed by the strict diagnostic laboratory sample handling standards. These include:
- CLSI phlebotomy guidelines.
- Laboratory accreditation standards of ISO 15189.
- Laboratory medicine evidence-based practices.
- Patient sample traceability system.
- Standardized labeling and tracking.
These standards ensure international consistency in test accuracy.
Best Practices in Pre-Analytical Error Reduction
The best practices that should be observed to minimize pre-analytical errors in labs to improve laboratory results are as follows:
• Train staff regularly
• Standardized collection tubes.
• Adhere to the order of draw strictly.
• Make sure that there is proper patient identification.
• Maintain aseptic conditions
• Monitor transport time
• Automated labeling systems.
These will help a lot in reducing the specimen rejection criteria and improving efficiency.
Conclusion:
Pre-analytical blood collection is not just a process involved in the testing process, but it is the cornerstone of laboratory accuracy. All the factors, such as venipuncture and sample transportation, have an impact on the final diagnosis. Following structured workflows, strict quality control, and reducing pre-analytical errors, laboratories obtain confidence in all the results they deliver.
TrustLab provides quality-oriented products to maintain precision and international standards by providing quality laboratory consumables and high-quality blood collection solutions.